Laryngotracheal Separation Surgery - Day 3
There have been a few post surgery issues to cope with that have made recovery not fun. No complications. Just not fun. Nathaniel's IV needed restarted. I have decided though it is a strong description, 'hate' is how I feel about the word occluded when it flashes from an IV machine. Thankfully Rich was here; he is always better at IV starts than I am. Nathaniel also has had some difficulty with voiding and has needed multiple catheterizations. Hopefully this minor issue will continue to improve.
We learned last week that our friend, Maverick, was traveling to Cincinnati and having surgery this week too. Maverick and Nathaniel were featured in a St. Louis Post Dispatch last spring when we met doing trach training for first responders. Maverick's room is four away from Nathaniel's room, and he came by this morning to share some toys. It was good to see Nathaniel smile during the visit. We have not seen many of those since Monday morning. When you pray for Nathaniel's airway, please pray for Maverick too. Everyone is hoping his surgery this week leads to getting his trach out later this year.
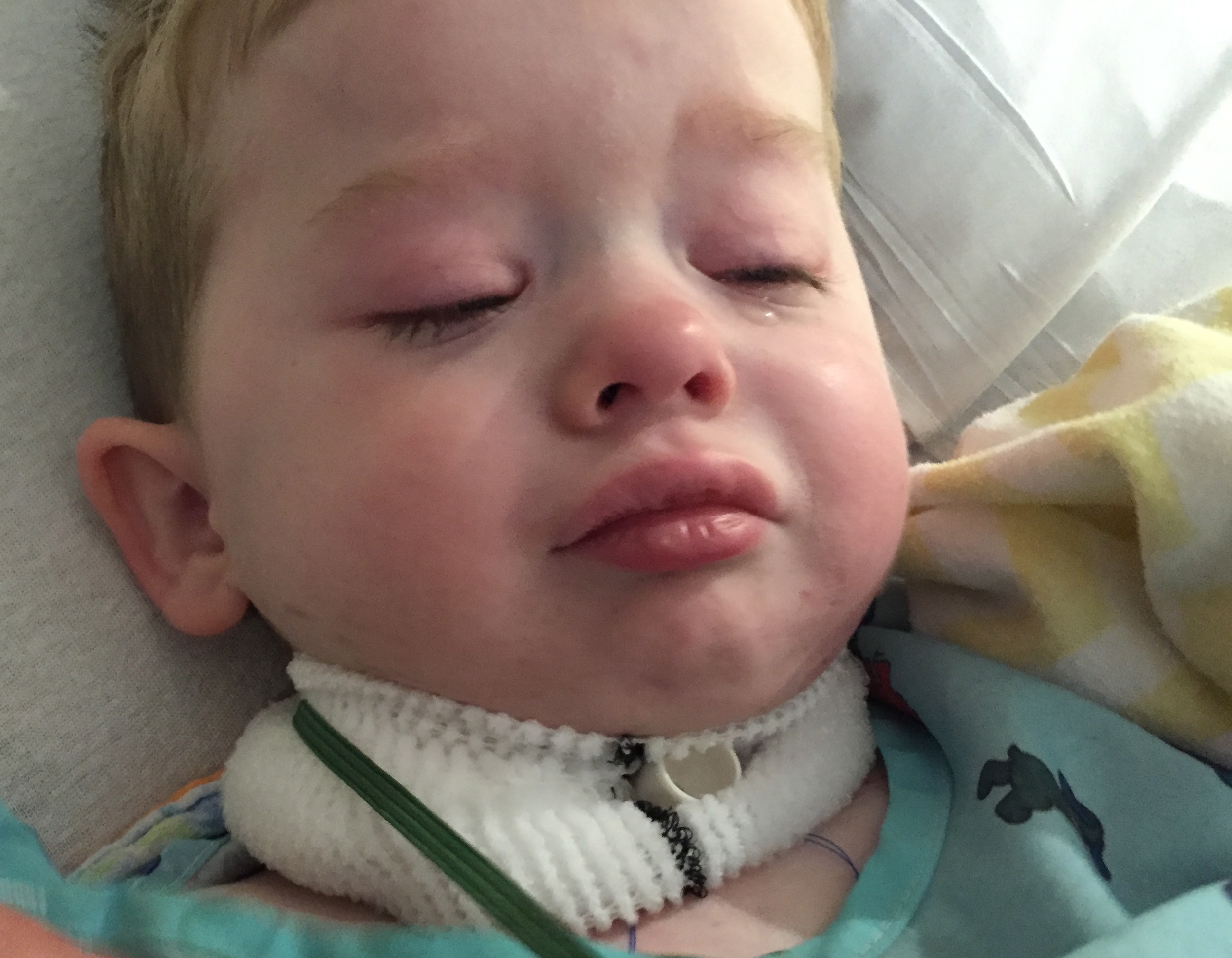
Sad photos, I know. It was a big surgery and recovery is slow. We do see progress. Tuesday he didn't want to be held. You might notice Nathaniel's trach tube looks different in these photos than before surgery. Nathaniel used to wear a Bivona FlexTend tracheostomy tube. The extended piece on the outside of the body was particularly helpful when he was an infant and toddler as there was not much room between the chin and chest. We are unsure exactly what type of tube he will wear on a regular basis now. It will need to be custom made as his larygectomy stoma is wider and lower than where his old stoma was positioned on his neck, thus requiring a shorter tube. The nurses have been providing daily cleaning of the stoma and dressings, but we have not changed trach ties since surgery. He has a drain that needs to come out first and then we will gradually increase to our home care routine. Rich and I will need to demonstrate competency and comfortableness with any new care before discharge, though we have been told by everyone it will be a piece of cake compared to what we are used to. Very interesting bit of info for anyone who likes medical stuff - peek back at the second photo above - the close up of Nathaniel's little sad face. The two blue strings coming out from under the dressing and going under his gown are taped to Nathaniel's chest. They are attached to his trachea inside the chest cavity. In the event that the suturing of the skin to the trachea would come undone, the trachea will want to retract down into the chest. The strings allow it to be pulled back up. Ewww... Cool... Blah... (These are temporary. They will be removed once the surface stitches are healed.)
The Critical Airway Unit has a sign outside the hallway doors: Quiet Please Our Airways are Healing. It is a shockingly quiet space for a hospital. All the rooms, called 'bedrooms' here, are private. Staff are quiet when they come and go. They talk soft. Little to no noise comes into the room from hall or nurses' station. It truly feels like a place where healing happens. Yesterday the floor nurse practitioner put her head in to check on Rich and me. Nathaniel was asleep, but she wanted to make sure we were ok and had what we needed. As we talked about post-surgery life for Nathaniel, she made the comment, "Probably by Jr. High he is going to have his own opinion about whether he wears a tube in his stoma or not. Most adults do not." Rich cracked a joke that with our strong-willed little guy, it will probably be earlier Jr. High. We all laughed.
I woke this morning at 3:00 am and her comment played over and over in my head. "When he is in Jr. High..." The comment marks the first time a medical professional has spoken to me of Nathaniel growing up. I have had a lot of conversations with a lot of doctors and nurses about Nathaniel in the last two years. While only small handful of those conversations were what I would describe as difficult, hard, or bad conversations, I often left appointments feeling sad, flat, and defeated. Even when everything I wanted to discuss was answered, when I received the congratulatory, "He is doing so well," pat on the back or fist bump, when they encouraged us to enjoy each day, it was not what I wanted to hear. Deep in my soul, I wanted to hear hope from the doctors and of the future they expected Nathaniel to have. Perhaps because of my love of words and language, I knew these were not future tense comments. Rather they were observations on Nathaniel's progress from the last appointment to the current one. They were comments about living now.
I do not fault the doctors for what they said at our appointments. The comments helped me get from one appointment to the next in hopes that I would hear of a long term plan or goal. They were happy and encouraging that we were doing all the right things for Nathaniel. But I knew the daily struggle of caring for Nathaniel well; I knew what we were doing, Rich and I as the only individuals comfortable with handling an airway emergency, was not sustainable for a decade into the future when Nathaniel would be in Jr. High. I realize today that for the past two years, it has not been what doctors said that always left me feeling discouraged, but what they did not say. Before coming to Cincinnati, there was no future tense. No plan. No middle school boy's strong will to laugh about. Proverbs sums it up well, "Hope deferred makes the heart sick."
Healing is happening at Cincinnati Children's Hospital Critical Airway Unit this week. Airway healing. Heart healing.
Continue reading about Nathaniel’s recovery here: Day 5
.